In life, we all lean on simple assumptions to make sense of complex systems.
They help us move faster. They help us explain what we’re seeing.
And sometimes… they quietly shape major decisions before we ever stop to question them.
One of the most common assumptions I hear in healthcare is this:
The clinicians carrying the heaviest workloads must be the ones most at risk of burnout and departure.
It sounds logical.
It feels obvious.
But as scientists, our job isn’t to rely on what feels obvious — it’s to test it.
So we did.
And the data tells a more complicated story.
This month’s Sisi’s Signals puts a big X through that equation.
We looked at clinicians across four quadrants:
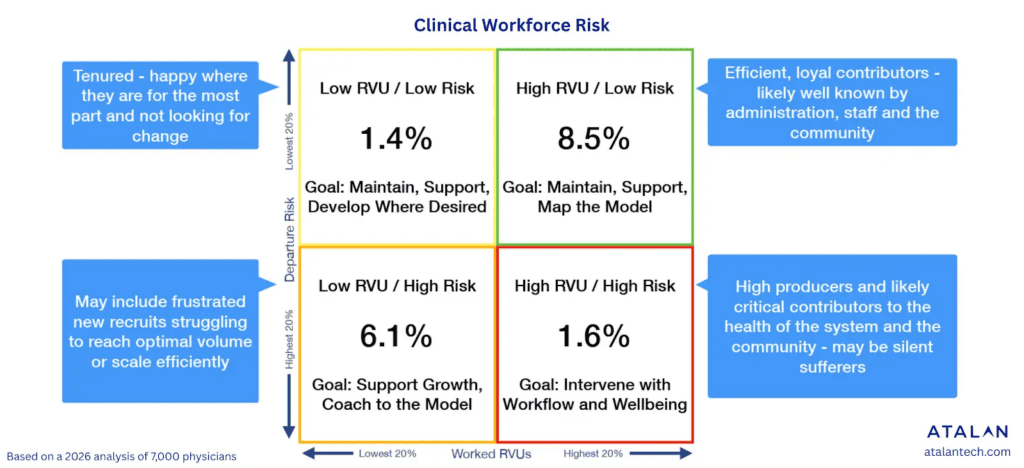
The data is clear. Many clinicians with high volume, high procedural intensity, and full plates are not at elevated resignation risk. At the same time, some clinicians with lower productivity are quietly approaching it.
Although workload may be a departure trigger for some, the evidence shows that it is not a factor for others. Workload is just one part of a much more complex tapestry of factors that impact each individual differently. Your clinicians do not provide the same treatment to every patient without understanding the individual. Similarly, health systems cannot expect results from broadly applied solutions in support of the clinical workforce.
This is exactly why our approach — what we call Clinician Retention Intelligence (CRI) — departs from check-the-box thinking. Retention risk isn’t something you can infer from a single trigger or solve with a one-size-fits-all fix. As tempting as it is to rely on assumptions, the reality is that the same signal can mean very different things in different contexts. High volume does not automatically mean “reduce workload.” Late-night documentation does not automatically mean “add AI scribing.”
CRI machine learning models analyze hundreds of signals together — including EHR usage patterns, scheduling dynamics, clinical intensity, tenure, compensation structure, role transitions, HR data, and beyond — to understand severity, combinations, and context. Two clinicians can look identical on paper and face very different levels of risk.
The result is a holistic, clinician-specific view of risk and recommendations that protect productivity instead of bluntly cutting it.
So here’s the reassurance many leaders need to hear:
Your highest-performing physician may be just fine.
And your real risk may be somewhere you’re not looking.
Only CRI data can tell the difference.
Xi (Sisi) Hu, Ph.D., Atalan Co-Founder and Chief Economist
