When we talk about clinician turnover, the conversation usually centers on how many clinicians are leaving.
But an important question is: when are they leaving?
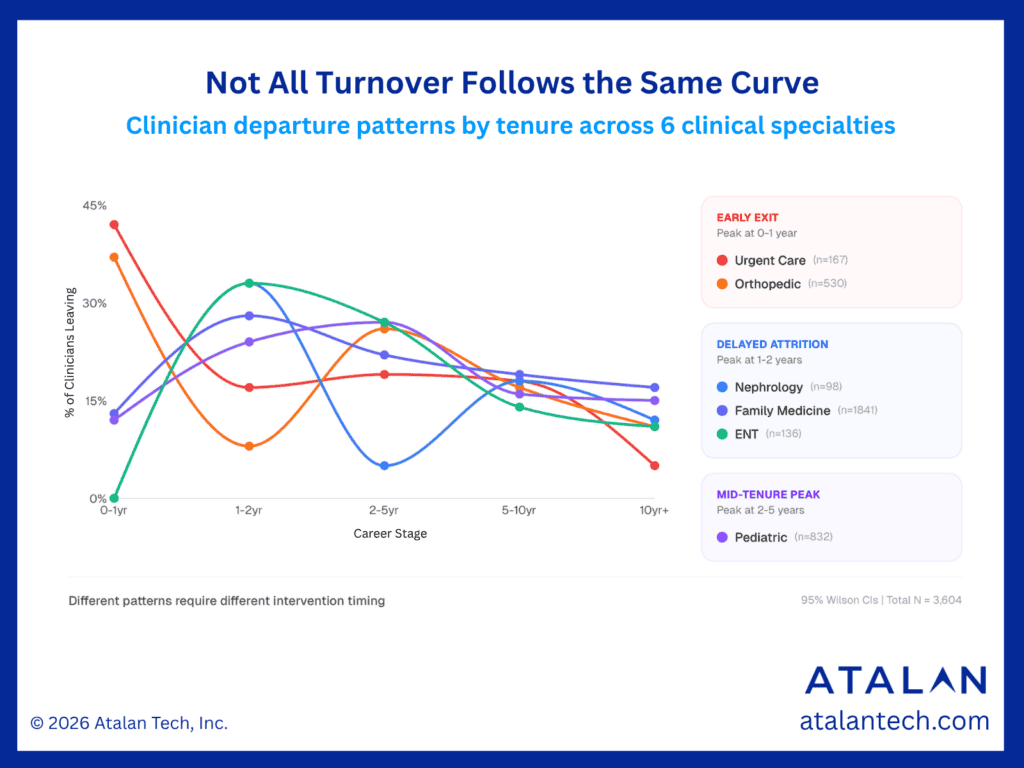
This week’s Sisi’s Signals looks at clinician departure patterns by tenure across six specialties, drawing on data from multiple health systems, and the differences are striking.
Some specialties show early exits, with turnover peaking in the first year. For example, urgent care reaches 43% of clinicians leaving in year 0-1, and orthopedics reaches 35% in that same window. These patterns often point to early-stage challenges: onboarding gaps, expectation mismatch, or immediate operational friction.
Others show delayed attrition, where risk builds over time. Family medicine (28%), ENT (32%), and nephrology (30%) all peak closer to the 1-2 year mark, suggesting pressures that accumulate after initial integration: workload sustainability, team dynamics, or system inefficiencies that compound over time.
And then there are specialties with a mid-tenure peak. Pediatrics (26%) reaches its highest level of clinicians leaving in the 2-5 year range, indicating a different kind of inflection point, often when long-term career decisions crystallize.
By the time clinicians reach the 5-10 year range, most specialties converge closer to 15% clinicians leaving and drop further beyond 10 years. In other words, the highest-risk window is often much earlier than many retention strategies are designed to address.
The takeaway: Turnover is not a single event. It’s a timeline. And that timeline varies by specialty and individuals.
Early-exit specialties require alignment from the start, beginning in the hiring process with clear expectations, team fit, role design, and early onboarding support.
Delayed-attrition specialties require sustained visibility into evolving strain.
Mid-tenure peaks require proactive career pathing and long-term alignment.
Treating all turnover the same means missing the moment where intervention is most effective.
With Clinician Retention Intelligence (CRI), these patterns become visible, allowing leaders to align interventions not just to who is at risk, but when that risk is most likely to emerge.
Consider it another signal, as we continue to explore what the data reveals upstream of clinician turnover.
