Most health system leaders are asking the same question right now: why are our clinicians leaving, and how can we make the leakage stop?
As a labor economist by training, for most of my career, I’ve focused on one question: how disruption and pressure in labor markets translate into real risk for workers – and for the organizations that rely on them.
I earned my Ph.D. at the University of Oxford and completed postdoctoral training at Harvard Law School’s Center for Labor and a Just Economy and the National Bureau of Economic Research. But more importantly, my work today is driven by a simple motivation: preventing clinician resignations so that health systems can protect revenue, and ultimately, improve care.
That’s why I’m introducing Sisi’s Signals.
Each month, I’ll share one scientifically grounded insight on Clinician Retention Intelligence (CRI) – a new category of healthcare technology that uses hospitals’ EHR and HR data and machine learning to predict exactly which clinicians are at risk of leaving. The intelligence also uncovers the reasons why and provides clear guidance to prevent unexpected resignations – before departures disrupt care or drain resources.
This month’s signal focuses on departure triggers. What actually pushes a clinician to resign?
Using machine-learning analysis of EHR and HR operational data from a multi-state U.S. health system with a few thousand physicians, we identified the most common factors associated with clinician departures at that specific health system and how frequently they affect physicians. In this visualization, each “bubble” represents a departure trigger, and its size reflects how many clinicians struggle with that issue.
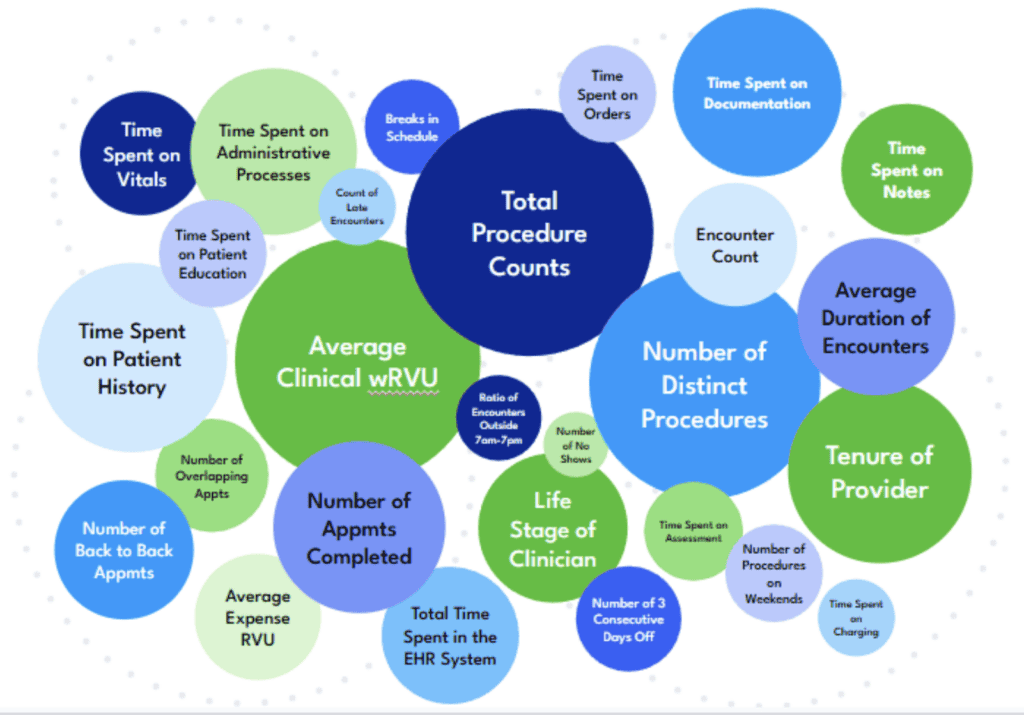
The large majority of these triggers are actionable and addressable by clinician leaders – if they’re aware of them.
At this health system, despite the adoption of AI scribes, documentation burden was a departure trigger for only 15% of physicians and did not rank among the top ten drivers of departure. In contrast, nearly 65% of physicians showed a departure trigger related to average clinical wRVU and 53% related to the number of distinct types of procedures. Other leading triggers include the number of back-to-back appointments, average encounter duration, and time spent on patient history. These are factors that add to cognitive burden, which are important to consider when assessing retention risk.
Documentation is often assumed to be a leading source of physician strain, but this example shows that it isn’t always the case. But there is no way to truly know without CRI.
If you knew these signals suggested that your top cardiologist was likely to leave within the next 12 months, what would you do differently today? What are the proven strategies you can deploy to better support your high-volume physicians without sacrificing access, throughput, or revenue?
That is the promise of CRI: not hindsight, but foresight – grounded in data, designed for action.
Are you surprised by the volume of any of these triggers? Are there any that are more or less than you expected?
Xi (Sisi) Hu, Ph.D., Atalan Co-Founder and Chief Economist
